|
6/20/2023 0 Comments Buddi health medical coding 
Based on RARC/CARC denial codes and automatically classified into respective denial work queues, an automated first-pass analysis is completed and then dropped into respective queues for experts, if needed, to conduct manual review prior to reappeal. AI Driven Denials Root Cause Analysis: Analyzes revenue leakage and reduces the lead time to get reimbursed for services rendered by eliminating the potential of manual error across the billing process, including explanation of benefits (EOB) root cause analysis. 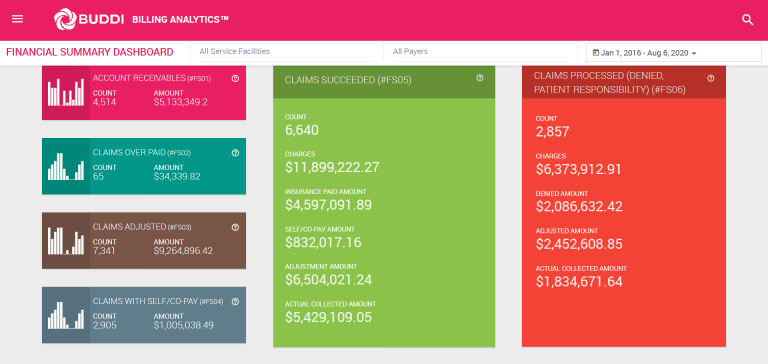
This real-time automation of the claims submissions process cuts down A/R times by 3X to 6X depending on the provider organization. Denial Prediction & Prevention | Claims Automation: Analyzes historical denials, approvals, patterns or other payer behavior based on both BUDDI AI and the institution's experience to proactively predict and prevent errors with claim submission, leading to reduced denials, faster A/R times and higher payer reimbursement.Medical Coding Automation: Automates structured and unstructured coding volumes-often the most burdensome function of RCM-with 95% or greater coding accuracy contractually guaranteed, to help reduce denials and increase reimbursements. 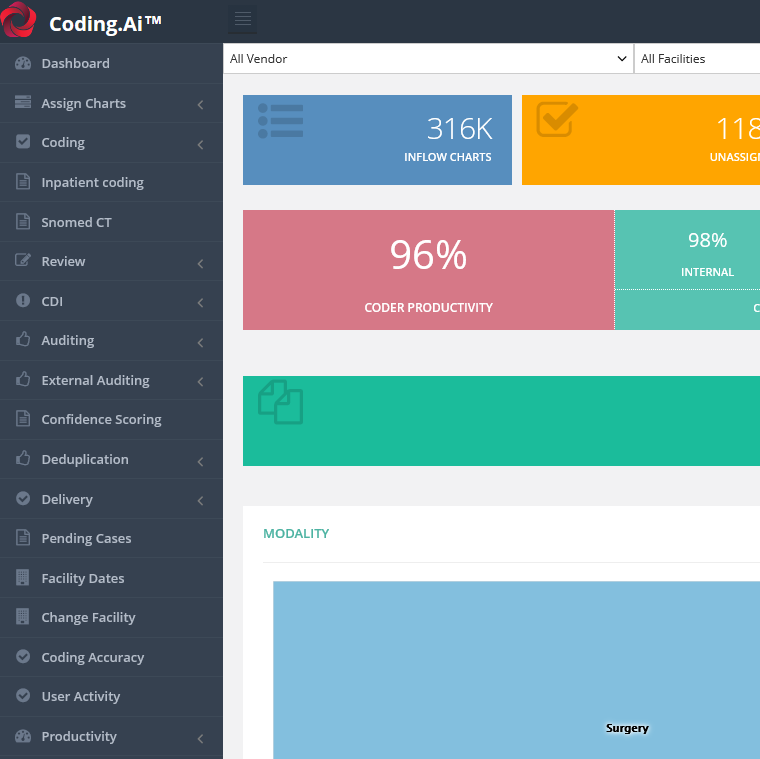
0 Comments
Leave a Reply. |

 RSS Feed
RSS Feed
